Homepage
Hospitals
Southampton General Hospital
Southampton General Hospital is the Trust’s largest location, with a great number of specialist services based here, ranging from neurosciences and oncology to pathology and cardiology.
Emergency and critical care is provided in the hospital’s special intensive care units, operating theatres, acute medicine unit and emergency department (A&E), as well as the dedicated eye casualty.
Southampton General also hosts outpatient clinics, diagnostic and treatment work, surgery, research, education and training, as well as providing day beds and longer stay wards for hundreds of patients.

Southampton General Hospital
Tremona Road
Southampton , Hampshire
SO16 6YD
Princess Anne Hospital
The Princess Anne Hospital is located on Coxford Road in Southampton, just across the road from Southampton General Hospital.
We are a centre of excellence for maternity care, providing a comprehensive service, including home birth, for about 5,000 women each year from around Southampton.
We are also a regional centre for fetal and maternal medicine, providing specialist care for women with medical problems during pregnancy, and for those whose baby needs extra care before or around birth.
Other services provided at the Princess Anne Hospital include genetics and breast screening.

Princess Anne Hospital
Coxford Road
Southampton, Hampshire
SO16 5YA
Southampton Children's Hospital
Southampton Children’s Hospital (SCH) leads the UK as one of the top three paediatric treatment centres.
We provide world class medical care for children across the south of England and further afield who are experiencing some of the most complex and severe illnesses and injuries. Part of University Hospital Southampton (UHS), one of the UK’s largest teaching Trusts, together we deliver transformative healthcare through pioneering treatment and research. Programmes that not only achieve many of the UK’s firsts in the field of children’s medicine, but also outstanding outcomes and lifetime care, from pre-birth through to end-of-life.
Our Centres of Excellence are led by specialist teams world-renowned for their expertise in cardiac, neurosciences, cancer, trauma and intensive care – in fact, we cover almost every specialism you can think of. Our doctors, nurses, therapists and wider children’s healthcare professionals have expertise in every childhood condition and offer continuity of care from diagnosis to treatment, rehabilitation and recovery. Working in partnership with our UHS colleagues in adult medicine we ensure that, where needed, we support our patients’ transition seamlessly into our adult care services on the same site when they reach 18.
The children we treat have always been and will always be our priority, but we extend that to the family that support them. We understand that caring for your child and ensuring the best outcome for them is a team effort, so we believe in supporting the family unit and bring you into our team to share decisions and shape your child’s care.
We hope you never need us but, if you do, know that you’re in the hands of one the best children’s hospitals in the country, possibly the world.
Leading research
We have a long and enviable history of being a research leader in children’s health creating a reputation that is built upon a longstanding partnership between University Hospital Southampton NHS Foundation Trust and the University of Southampton. The partnership proudly hosts a National Institute for Health and Care Research (NIHR) Southampton Clinical Research Facility and a Biomedical Research Centre.
We run hundreds of studies at any one time spanning a wide range of conditions, such as cystic fibrosis, inflammatory bowel disease and rare lung conditions. Researchers are also exploring how asthma and allergy can be prevented from an early age.
This means that our patients have some of the best access to new therapies and technologies in the country. This includes ground-breaking cancer treatments.
Together with our research partners, we are improving treatments and care through research and helping to transform children's lives.

Southampton Children's Hospital
Southampton General Hospital
Tremona Road
Southampton, Hampshire
SO16 6YD
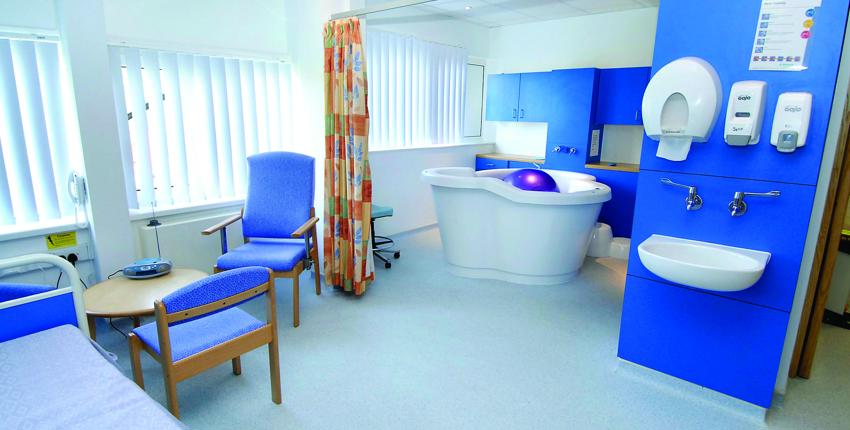
New Forest Birth Centre
The New Forest Birth Centre is at Ashurst on the edge of the New Forest.
Run by experienced UHS midwives and support staff, the New Forest Birth Centre offers a safe, friendly environment for you and your baby.
The birth centre also provides antenatal support in preparation for parenthood, private spaces and ongoing support including breastfeeding support groups.
New Forest Birth Centre
Ashurst Hospital
Lyndhurst Road
Ashurst , Hampshire
SO40 7AR
Royal South Hants Hospital
Services at Royal South Hants
The Royal South Hants Hospital is located near the centre of Southampton and is managed by NHS Property Services Ltd.
A small number of UHS services are provided here.
Urgent Treatment Centre
The Southampton urgent treatment centre is also based at Royal South Hants and is run by Practice Plus Group.
Find out more about the Southampton UTC here on their website.
Address
Royal South Hants Hospital
Brintons Terrace
Southampton
SO14 0YG
023 8054 0087
Getting here and parking
The NHS website provides further information about parking and public transport for the Royal South Hants.

Royal South Hants Hospital
Brintons Terrace
Southampton , Hampshire
SO14 0YG
Lymington New Forest Hospital
Lymington New Forest Hospital is a community hospital located in Lymington and managed by Southern Health NHS Foundation Trust. UHS manages surgical services at the hospital.


Surgeons: At the Edge of Life episode 5
The gripping series Surgeons: At the Edge of Life continues tonight showcasing the talent and skill of our incredible teams at UHS as they carry out some of the country’s most challenging operations.
In tonight’s episode we meet 70-year-old grandmother Jeanette who is in desperate need of heart surgery as her aorta could rupture at any moment – an often-fatal situation.

Our Services

The Trust provides a wide range of healthcare services for Southampton, central southern England and the Channel Islands.
Search for the service you’re looking for