Hospital trust's pioneering kidney cancer work reflected in new national guidelines
Doctors at University Hospital Southampton (UHS) who pioneered the use of a revolutionary non-surgical treatment for kidney cancer have welcomed new NICE guidelines which recommend it should be rolled out across the NHS.
The treatment, known as thermal ablation, is a minimally invasive technique that uses image-guided needles or probes to destroy cancerous or abnormal tissue by applying extreme temperatures – either heat or cold – directly to the site of a tumour.
As it is less invasive and avoids damage to surrounding healthy tissue, most people experience far less pain, a quicker return to normal activities and a much shorter recovery time compared to traditional surgical options – with similar outcomes.
Kidney cancer is the sixth most common cancer in the UK, with around 13,900 new cases diagnosed each year. Incidence is also rising among younger adults, highlighting the importance of early detection and timely access to treatment.
The new guidance, published today (Thursday, 19 March), forms part of wider national efforts to improve access to evidence‑based cancer therapies and ensure better outcomes for patients.
After reviewing safety, efficacy and cost data, NICE – the National Institute for Health and Care Excellence – determined thermal ablation is associated with fewer short‑term complications than surgery and offers improved preservation of kidney function.
The approach is also suitable for individuals who are not fit for major surgery or who have only one functioning kidney – and many patients are able to go home the same day.
Southampton’s image‑guided ablation service, established in 2001 and now marking its 25th anniversary, has grown into a national leader, training almost all major UK centres in cryoablation and contributing significantly to the development of microwave ablation services.
Cryoablation was pioneered at UHS in 2008 by consultant abdominal radiologist Dr David Breen – and Southampton remains at the forefront of CT-guided ablation within the UK for kidney and liver tumours.
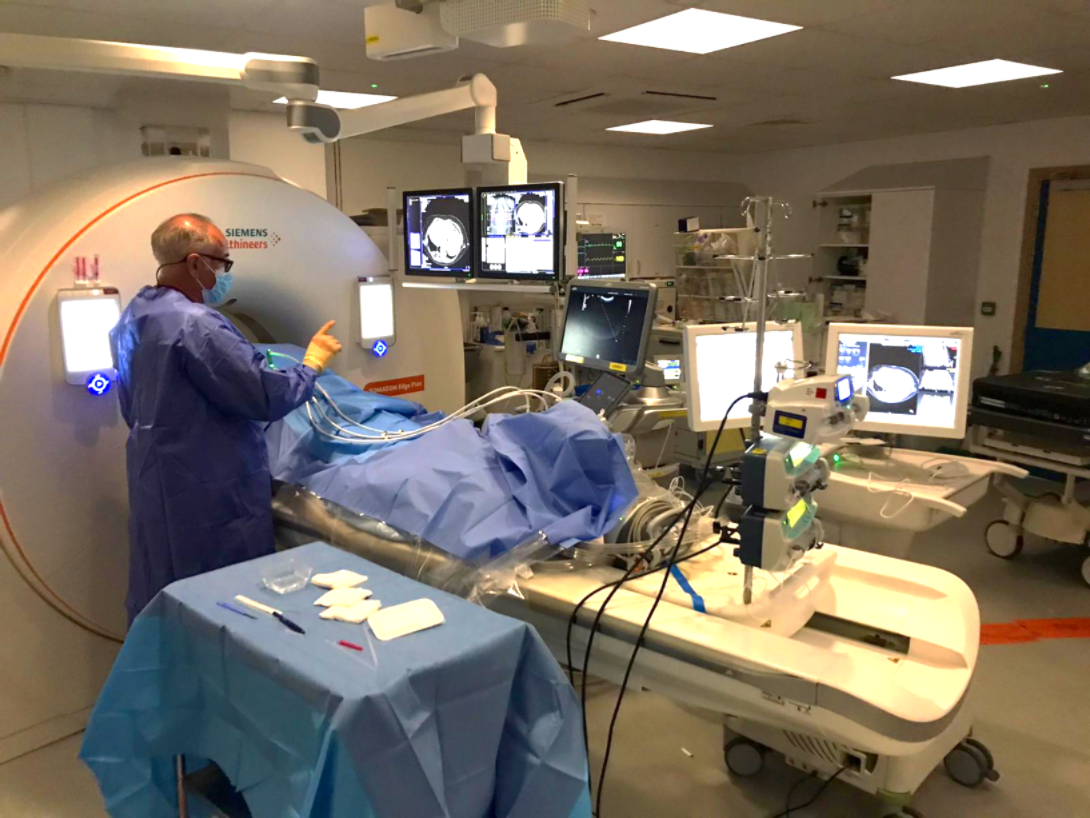
UHS currently runs the UK’s only MRI‑guided cryoablation service, offering advanced treatment options for tumours in the kidney, liver, lung and other sites.
It uses extreme cold to target tumours and, importantly, can be repeated if needed, offering ongoing treatment options for the very few patients whose tumours recur or who develop new lesions, while surgery can only be performed a limited number of times.
Cryoablation is commonly used to treat small renal cell carcinomas (RCC), the most common type of kidney cancer, and is frequently carried out as an outpatient alternative to surgery.
The technique also has wider benefits by reducing pressure on surgical theatres and inpatient beds, with shorter stays improving patient flow and fewer complications reducing follow‑up care needs.
UHS serves as a major UK referral hub for kidney cancer ablation, regularly managing complex cases that cannot be treated locally. To date, the team has carried out more than 1,000 procedures, placing the Trust among the highest‑volume specialist centres in the country.
The Trust is also recognised as a national European leader in thermal and cryoablation for kidney cancer, led by the pioneering work of Dr Breen and fellow consultant radiologist Dr Alex King, along with other UHS colleagues.
The team has treated one of the largest patient cohorts in Europe and produced key evidence showing that minimally invasive freezing techniques can achieve outcomes comparable to surgery, but with faster recovery.
Their landmark 2018 Radiology study of 220 patients with biopsy‑proven renal cell carcinoma reported a 94% five‑year recurrence‑free survival rate – results on par with partial nephrectomy and central to informing the new NICE guidelines.
In addition, their research has also demonstrated that cryoablation is effective for both small tumours and larger lesions up to 7cm.
The UHS team plays a key role in the European Renal Cryoablation (EuRECA) Registry, ensuring UK patient data contributes to international research helping to shape global practice in kidney cancer care.
David Stanley, 75, from Guernsey, underwent cryoablation at UHS in 2024, helping him overcome kidney cancer with minimal side effects.
He said: “Given my circumstances and the previous procedures I’d had, cryoablation was very much recommended as the most suitable treatment for my kidney cancer. The procedure itself made very little impact on my daily life – I recovered ever so quickly.”
His procedure was carried out by a team led by Dr King, who used a CT scanner to guide the needles, or cryoprobes, into the tumour while minimising impact on surrounding anatomy.
Dr King said: “Cryoablation has transformed the way we treat small kidney tumours. Using real‑time imaging, we can precisely target the cancer while protecting surrounding renal tissue and other vulnerable structures, meaning patients recover faster and can avoid some of the risks of major surgery.
“We are proud that our research and clinical outcomes have helped shape the new national guidelines, and we hope this will lead to wider access to safe, effective and patient‑friendly treatment options across the NHS.”
Dr Breen added: “These new NICE guidelines recognise the enormous progress that has been made in minimally invasive kidney cancer treatment.
“Cancers are getting smaller at the time of detection, almost entirely due to scans and radiology - and this is driving the push from open to laparoscopic and on now to image-guided surgery.
“Thermal ablation allows us to remove tumours safely while preserving as much kidney function as possible – something that is particularly important for older patients or those with other health conditions.
“Southampton has been a trailblazer in this field and, after more than 15 years of offering this service at UHS, it is extremely encouraging to see the evidence now reflected in national guidance so more patients across the country can benefit.”