Study of mechanisms of action of omalizumab in severe asthma (SoMOSA)
We're looking for participants with severe allergic asthma to take part in a study to better target use of the treatment Xolair (omalizumab) to those it will benefit most.
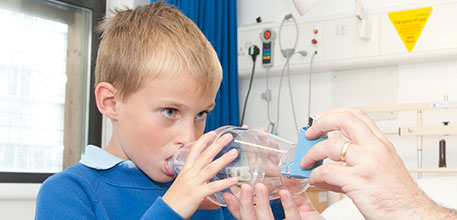
Treatment with Xolair
Xolair (omalizumab) has been shown to be very effective at reducing the number of episodes of worsening of asthma (exacerbations), and to enable reduction of steroid doses, reducing side effects and improving patients’ quality of life.
However some patients benefit more than others, so we are aiming to predict which patients Xolair will help the most. We're doing this by identifying ‘biomarkers’ (biological substances that change in response to disease or treatment), associated with a good response to Xolair.
Taking part in severe asthma research
If you have severe asthma, you can take part in any of our studies aimed at improving management of the condition, including the Xolair study.
One of our team will discuss the research with you and if you are happy to proceed, we will ask for your written consent. We then perform some tests to ensure you are suitable for the study and that you are fit enough to participate. These tests include:
- Skin prick test: We will place drops of allergens on your skin to see if allergic reaction appears. This is to confirm that you are allergic. Emergency care is available if needed to treat rare cases of a whole body reaction.
- Sample tests: In order to prescribe the appropriate dose, a blood test will be required (3 teaspoons) for a routine health screen. You may not need to provide a sample if you had a blood test within the last 3 months before your visit. This test can cause some discomfort. Also a urine and a sputum sample will be collected. The sputum induction process will require you to inhale different strengths of a salty mist.
- Electrocardiogram (ECG): This test will be performed to check your heart electrical activity. Self-adhesive electrodes will be attached to selected location on your arms, legs and chest.
- Vital signs: This includes blood pressure and temperature. Height and weight will also be measured.
- Pulmonary function test: You will be asked to blow into a machine to measure the amount of air you have in your lungs (spirometry). We may have to perform a reversibility test including a spirometry test followed by some puffs of your blue inhaler (normally ventolin) and wait for 15 minutes before repeating a spirometry again. This will give us an indication of how well you respond to your blue inhaler.
- Exhaled Nitric Oxide: The amount of nitric oxide can be used as a guide to diagnosing and treating asthma. You will be asked to blow into a mouthpiece at different speeds.
- Breathomics: You will be asked to breathe into a bag and the gas exhaled will be analysed.
- Cotinine testing: As smokers are not allowed in the study, this test is done in smokers/ ex-smoker by taking a sample of urine.
- Pregnancy test: Where applicable you will be asked to provide a urine sample to check whether you are pregnant.
We will also ask you some questions about your asthma. Details about your medical history will also be recorded in strict confidence.
If you’re interested in taking part or you would like to get further information and assistance, please contact our respiratory research nursing team on 023 8120 4479/ 023 8120 8427 or email