Orthopaedic surgeons in Southampton have said selective screening introduced in 1986 to identify hip problems in babies in England has "failed" to prevent late diagnoses.
Currently, babies receive an ultrasound only if potential developmental dysplasia of the hip (DDH) is found on physical examinations around the time of birth or at six weeks, or if the infant has specific risk factors.
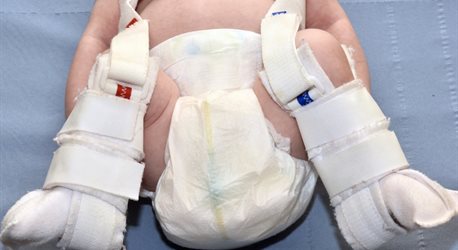
If detected early in infancy, the problem can be treated by a removable splint worn for two to three months to stabilise the position of the hips and help them develop normally, with 95% success rates.
However, if diagnosed after three months, it is associated with an increased number of invasive operations, longer hospital stays, greater healthcare costs and long-term complications.
In landmark research published in The Bone and Joint Journal, doctors at Southampton Children's Hospital found the incidence of late-diagnosed DDH remains similar to the figure recorded 35 years ago prior to the introduction of the current national selective screening programme.
"Hip dysplasia is a significant public health issue which, untreated, represents the single largest cause for arthritis and total hip replacement in young adults,” said Alexander Aarvold, a consultant orthopaedic surgeon at Southampton Children's Hospital and study lead.

“Detection in children over one year of age remains a persistent reason for referral to paediatric orthopaedic units.
“This is despite the introduction of selective screening introduced in England in 1986 as part of the Newborn and Infant Physical Examination (NIPE) programme, so there are searching questions for Public Health England (PHE) regarding the impact, if any, of selective screening on the prevention of late diagnoses.”
The study of almost 15 million patients, the largest population study on DDH and the first to use linked primary and secondary care records, examined national records of all children from 1 January 1990 to 1 January 2016 who were diagnosed between one and eight years old.
The overall incidence of late diagnosis within England of 1.28 per 1,000 live births is greater than previously reported 37 years ago in Southampton (0.47) from 1965 to 1978 and 34 years ago in Bristol (0.39) from 1970 to 1979.
If not picked up in infancy by screening, the problem is usually detected after the child starts walking. These children all need surgery to get the hip into joint and reduce the chance of arthritis in young adulthood, as opposed to being treated in a splint if detected earlier.
“The approach of selective screening appears to have failed to impact on incidence rates of late-diagnosed DDH and it remains a still uncontrolled disability across the country,” said Mr Aarvold, who presented the findings at the British Society for Children's Orthopaedic Surgery (BSCOS) conference.
“In contrast, countries such as Austria and Germany undertake universal screening by performing an ultrasound scan of the hips of all newborns. In these countries, the incidence of late-diagnosed DDH is low, with little requirement for surgery and fewer hospital admissions.
“How to optimise the screening programme for infant hip dysplasia is one of the top research priorities for the BSCOS. This can inform PHE as to the optimal means to screen for DDH and to identify if implementing universal screening at a national level will effectively reduce the societal burden of this disability."
Tim Theologis, president of the British Society for Children's Orthopaedic Surgery, said: “This study has provided evidence that the current selective screening for neonatal hip dysplasia is ineffective and the percentage of infants diagnosed late is unacceptably high.
“There is a pressing need to present convincing evidence to policy makers for the neonatal hip screening guidelines to change and BSCOS will fully support this effort.”
*Image courtesy of https://www.nhs.uk/conditions/developmental-dysplasia-of-the-hip/
Posted on Friday 29 March 2019